
250 mtrs opp, Neo Majestic Hotel, Alto Porvorim, Goa 403521

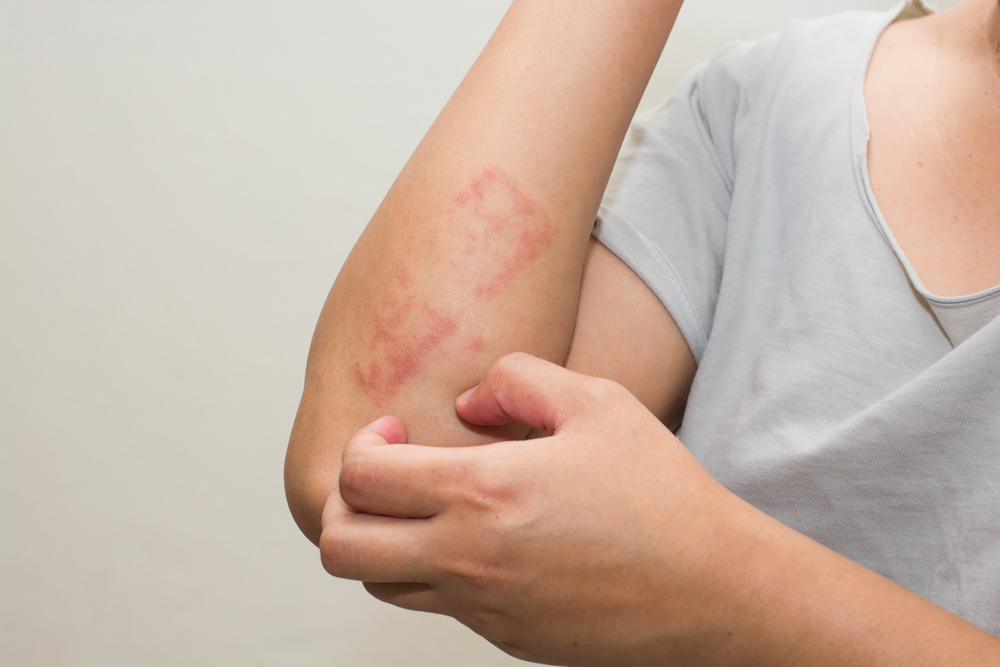
Urticaria is a vascular reaction of the skin marked by transient appearance of smooth, slightly elevated patches that are often associated with severe pruritus. In simple words it is a rash that itches and lesions always last for few hours and never more than 24 hrs. Although new fresh lesions can appear and course of this condition can last for few days to months.
Angioedema is au condition when deep skin tissues are also affected which may take over 24 hours to clear, usually there is no itching and can affect the lips and tongue. Some patients have one or the other condition, others have both.The most common form of urticaria is spontaneous urticaria. In this type no cause is usually identified.
Urticaria is usually divided into ‘acute’ and ‘chronic’ forms. Inu ‘acute’ urticaria, the episode lasts up to six weeks. It is usually a self limited illness requiring little treatment other than antihistamines.

Chronic urticaria, by definition, lasts for more than six weeks, requires specialized consultation and full work up from qualified allergist for proper scientific management of this debilitating disease.
Urticaria is caused by the release of histamine from cells in the skin called mast cells.Often a specific cause cannot be found. Sometimes an infection such as a cold can be a trigger. Other triggers include physical contact with an allergen such as anu animal, sun exposure or a specific food or medicine. For young babies, in whom it is rare, cow’s milk allergy is the commonest trigger. Bee and wasp stings can trigger urticaria, as can eating shellfish, nuts, apples, peaches etc. Almost any medicine can cause urticaria, but painkillers (especially aspirin and medicines like ibuprofen), antibiotics (especially penicillins), blood products and vaccinations are most likely to be responsible.
Angioedema, in particular, can be caused by a type of drug (ACE inhibitors) used to treat high blood pressure.
In some patients with chronic urticaria, the release of histamine from skin mast cells is triggered by factors circulating in thej blood, such as antibodies directed against their own mast cells - a process known as autoimmunity which requires some specific tests for diagnosis like Serum Anti Nuclear Antibody or Autologous Serum Skin Test. Urticaria rash quite frequently occurs in Autoimmune thyroiditis. In this condition thyroid antibodies can be positive.
Chronic Urticaria is often thought to be due to allergy, but in fact very rarely specific allergen is found to be a definite causative agent for urticaria symptoms.
Chronic Urticaria or repeated rashes and wheal that last more than 6 weeks can have reasons other than allegens also as causative factor. Various autoimmune conditions in which one's own immunity reacting to yourself can be one of the cause.
*Symptoms of urticaria and angioedema:*
The main symptom ofu urticaria is itch. Angioedema is usually not itchy but may be painful. Although urticaria can be distressing, because of the itching and its appearance, it has no direct effect on general health. Rarely, the swelling of angioedema may affect the tongue or throat, causing difficulty with breathing or swallowing. This can be alarming but is rarely life-threatening.
Although urticaria rash may persist for many weeks or months, individual lesions typically disappear within a day, and often last only a few hours. New wheals may then appear in other areas. In spontaneous urticaria, wheals can occur anywhere on the body, at any time.
The deeper swellings of angioedema occur most frequently on the eyelids, lips and sometimes in the mouth, but they may occur anywhere. They are usually not itchy, and tend to last a few days. The skin may feel tight and painful.
*How is chronic urticaria diagnosed?*
Usually its appearance, or a description is enough for you to make the diagnosis. In the vast majority of people no cause can be found even after knowing detailed history. There is no single test that is available which can reliably identify the definite cause of urticaria. Occasionally, if a trigger is suspected, a specific blood test, to detect antibodies in the bloodstream, or a skin prick test may be performed by qualified & experienced Allergist.
In a small percentage of people, foods, or it'scolouring agents and preservatives appear to worsen urticaria, and it might be helpful to identify these by keeping a food diary. These substances can be left out of the diet to see if the condition improves, and later reintroduced toconfirm whether they are the cause of the urticaria. However, as urticaria is such a fluctuating disease, this is not always accurate and will not always show you definitely what is causing the problem.
*Treatment of Urticaria*
The treatments outlined below suppress the symptoms of the condition rather than cure it. In about half of the people affected by chronic ordinary urticaria, the rash lasts for 6-12 months, and then gradually disappears. It can however last considerably longer.
In any one individual the course of urticaria is unpredictable.Antihistamine tablets block the effect of histamine, and reduce itching and the rash in most people, but may not relieve urticaria completely. If urticaria occurs frequently, it can be helpful to take antihistamines regularly every day.
There are many different types including non-sedating and sedating antihistamines, as well as short acting and long acting types. The antihistamine tablets has to be taken for as long as the urticaria persists. Even the non-sedating types can make some people sleepy, and as with all medications there can be side effects; the balance of risk and benefit needs to be considered when taking these and all treatments.
2nd Generation Non sedating H1 antihistamines like levocetrizine or fexofenedine dose can be increased to 2 folds if not controlled with normal dosage. They are generally safe and are well studied even for long term use in children up to 18 months at a stretch but at every 3 months needs to be given break to see if patient is gone in spontaneous remission. Please note if long term antihistamines are required all possible treatable causes are ruled out by all investigations as per standard guidelines.
A new biological monoclonal antibody omalizumab has recently been approved for the most severely affected antihistaminic resistant chronic spontaneous urticaria patients.
It is important to avoid anything that may worsen urticaria, such as heat, tight clothes, and alcohol. Triggers vary between individuals.Avoidance of specific foods, colouring agents and preservatives may be helpful wherever these have proved to be a problem. Stress is being found as a major trigger factor for cronic urticaria in recent times even in children. Exam stress with no relaxing activity in between is being noticed specially in adolescent children studying hard for competitive exams. Lifestyle changes are advisable in these patients and quite frequently relief is found.
*Other types of urticaria:*
In some patients, clear trigger factors for urticaria can be identified; these are called inducible urticarias. There are several types of inducible urticaria.
*Physical urticarias -* Urticaria may be triggered by heat, cold, friction, pressure on the skin and even by water. The wheals usually occur within minutes, and last for less than one hour (except delayed pressure urticaria). Physical urticarias is usually occur in healthy young adults, and are not uncommon.
Some patients suffer from more than one type of urticaria; they include the following types:
*Dermographism* (“skin writing”)-In this type, itchy wheals occur after friction such as rubbing or stroking the skin. Itch may be aggravated by heat. Wheals and red marks often appear as lines at the sites of scratching, and generally last for less than an hour.
*Cold urticaria.*- This is triggered by exposure to cold, including rain, windu and cold water, causing itchy wheals. Swimming in cold water may cause severe wheals and fainting, and should be avoided. Patients should report their cold urticaria to medical personnel before operations so that, if wheals appear during the procedure, cold urticaria can be considered.
*Solar urticaria.*- This is rare. Redness, itching and wheals occur on the skin immediately after exposure to sunlight, and last for less than one hour after avoidance of exposure.
*Aquagenic urticaria.*- This is extremely rare. Small wheals occur on the skin at the site of contact with water, usually on the upper part of the body.
*Delayed pressure urticaria.*- usually develops where pressure has been applied to the skin, for example from tight clothes or from gripping tools. Usually the swelling develops several hours later. It can be painful and last longer than a day. People with pressure urticaria nearly always have ordinary urticaria as well.
*Cholinergic urticaria* - This occurs under conditions that cause sweating, such as exertion, heat, emotional stress and eating spicy food. Within minutes, small itchy bumps with variable redness appear, usually on the upper part of the body but they may be widespread. The wheals last for less than an hour, but in severe cases may join together to form larger swellings. Antihistamines usually help, and are sometimes best taken before a triggering event (e.g. exercise).
*Contact urticaria*- Various chemicals, foods, plants, animals, and animal products, can cause wheals within minutes at the site of contact. These do not last long. Some of the commoner causes are eggs, nuts (e.g. peanuts), citrus fruits, rubber (latex) and contact with cats and dogs. Although often the reactions are mild, occasionally they can be severe, for example after contact with rubber and peanuts in very sensitive individuals.
Many spontaneous urticaria usually improves by avoiding their trigger, and by taking regular antihistamines. Delayed pressure urticaria can be more difficult to treat.
Sometimes a short course of oral steroids will help if the symptoms of delayed pressure urticaria are very severe. Angioedema without wheals - Angioedema occurring without urticaria can be due to medicines (e.g. aspirin, ACE inhibitors) or food allergies. When angioedema occurs without wheals, a hereditary form of angioedema should be considered.
*Hereditary angioedema* : Although histamine induced angioedema is much common one should be aware of a very rare form of bradykinin induced angioedema which tends to run ini families.
Patients have intermittent swelling of the face, mouth, throat, and sometimes of the gut, leading to colic. The condition is due to an inherited deficiency of a blood protein C1 INH and can be identified by a blood test.
When suspected Serum C3, C4 should be done and if you find low level further diagnostic test C1 INH both function and level should be ordered. It is usually resistant too antihistamines, steroid and adrenaline which works in histamine induced Angioedema.
One needs to replace deficient protein C1 INH concentrate. But since it is not easily available, fresh frozen plasma has to be given. This should be kept in mind specially when patient does not respond to antihistamine, steroid and adrenaline since a severe attack of hereditary angioedema can be life threatening if left untreated.